 This is the the hardest story that I am living, and the most difficult one to write about.
This is the the hardest story that I am living, and the most difficult one to write about.
I knew I wanted to share this part of my pregnancy with you too, because it is real and true and heartbreaking and a part of my life that I cannot ignore or deny.
But I am conscious that it is not only my story to tell. It is also my husband’s story, and his comfort is mine and his pain is also mine. So it is only with his permission that I share this with you today.
We had to say goodbye to our sweet baby girl at 6 months of pregnancy.
At my 20 week anatomy ultrasound scan, we were told our baby was falling behind in growth. My OB was concerned and referred us to a high risk maternity clinic for further investigations. At the time, we were not worried. I am a petite woman, and I never expected to grow a big baby.
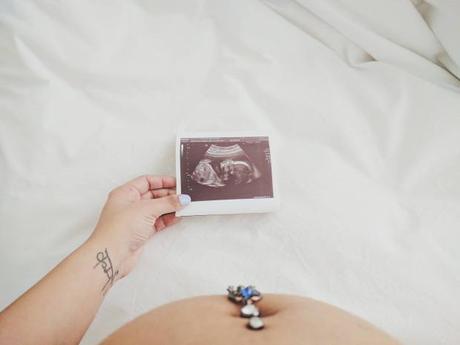
The day we went for our follow up appointment was a bright warm February day. The warmest February day in Toronto – my husband tells me. We were concerned, naturally, but we were mostly optimistic. 15 minutes into the scan, the doctor joined us and took over. The atmosphere changed and it was clear something was not right. Because of my medical back ground, I knew things did not look good for us, but I didn’t know the extent of it.
We spoke to the doctor afterwards in his office and everything was a blur. There was a heaviness in my heart, a lump in my throat. It was hard to speak, to think, to understand what was happening.
Intrauterine Growth Restriction (IUGR) due to placental insufficiency.
My placenta was functioning at only 30% of its capacity. Our baby had been severely deprived of the oxygen and nutrients she needed to grow and survive.
The flow from my placenta to my baby was intermittent absent. Not good. Not the worst. But not good.
We don’t know why this happened. There was nothing in my medical history to indicate a cause. But of course, more specific investigations are being planned to find out what happened. What went wrong.

I was 23 weeks pregnant at the time, a week shy of completing 6 months of pregnancy. Our babygirl was entering the “Grey zone” of viability. A baby is said to be viable at 24 weeks gestation – which means that with the help of medical intervention, they can survive outside the womb. They are of course, at risk for all the complications of an extremely premature birth, but medicine has advanced so much that specialized neonatologists have plenty of tricks in their bag to help the baby live.
The problem was, while she was 23 weeks according to her gestation, due to her condition (IUGR), she was actually only 19-20 weeks. Still not viable. Can’t survive. Not yet.
315 grams. The doctors tell us that they have not yet been successful with a baby this premature and this small. But that every week in pregnancy can make a difference.
The management for IUGR babies is to plan a premature delivery. The question is when. Our problem was double fold. Not only will she be premature, but she is also growth restricted. There was no point to intervene and do an emergency c-section now as there was no chance that she would survive when she was this tiny.
So we were going to wait. We were going to come back next week to see if the baby has grown. If she could just make it to at least 500 grams, maybe she has a chance. Maybe she could live.

We went home. I cried all day and my husband held me. I am so disappointed in my placenta making abilities. I feel so deeply disappointed that my body failed my baby. I was inconsolable.
Over the week, we went through a whirlwind of emotions, but as the days went by, I started to feel hopeful. Our baby can grow. I read many stories of other women with babies in similar circumstances, and many of them made it. There was hope.

That week felt like a long dark year. When we went for our follow up scan, the conditions for my daughter in my womb had only deteriorated. She had not grown enough. We also now had continuous reversed diastolic flow through the arteries from my placenta to my baby. This is not a good sign, in fact it is one of the last signs, and usually indicates immediate intervention to do an emergency c-section and take out the baby before she passes away.
There were a number of serious medical risks that would not allow me to have a c-section.
Because my uterus and baby was still so small, they would have to cut into the muscular part (the wrong part) of my uterus, which would put me at high risk for fatal (for both myself and the baby) complications in future pregnancies such as uterine rupture. The internal scarring would also make it difficult for us to conceive again in the future.
Our doctors were excellent and we met our OB and a neonatologist who sat with us and talked to us, and never once rushed us. It was like an out of body experience, hearing the words coming out of their mouth. Like watching myself trapped in a bad dream. Like a trap door at the bottom of my heart that was pulled from beneath me and I’m falling.
In medical school, we are taught how to break bad news to patients. And yet, it could not prepare me for being the recipient of it.
In the heart of the moment, everything fades away, and all I realize is how truly important it is, how much it helps to know how to talk about loss and heartbreak to a complete stranger. How the way they spoke to me mattered, at times even more than what they were saying.
Coming from a medical background I already I knew that things did not look good for our babygirl. But I was scared of having a list of awful statistics dumped on us. Statistics – the language of bad news. I was afraid of the numbers.
But our neonatologist didn’t give us any statistics. And I was glad for it. My husband asked for them, because the internet is full of them, and we wanted to put a number, a percentage, on our suffering.
But the doctor said “I don’t talk about statistics. What’s the point? If I give you a number, you will cling to that number but it doesn’t mean anything. If I tell you the chance that your child will have a certain condition is 1%, and yet your child gets that condition, then it’s 100% for you.”
I appreciated that. I didn’t want the future of our daughter written out in numbers. She is not a statistic to us.

But, having said that, the prognosis was not good. In fact, it was pretty awful.
On Monday the 6th of March, we said goodbye to our baby girl. It was the deep dark center of heartbreak. And on Thursday the 9th of March, I delivered our sleeping girl.
Nameless
We did not want to name our daughter. I know that many parents in our situation wish to do it to honor their child, but for us, neither of us felt we wanted to do it this way.
What is a name? A name is something we use in society so that we can identify someone, so that we can call them and they will know it is in reference to them.
Our daughter will never live in our society. Not in our world. Naming her almost felt like limiting her, putting a label on who is she is to us – a label that could never do her soul and her presence in our life justice.
She is our nameless wonder.
So expansive.
When I talk about her, I call her my angelbaby. And to our close friends and family who love her as deeply as we do, a name never felt necessary. She is our child. Our baby. Our angelbaby.
After she was born and died, we had to register her birth and death. For this, we needed a name.
So we decided to name her Mia.
Short, and sweet, like her life.
The latin meaning for her name is – a wished for child.
This post is already very long, so I have split it into two posts. In the next post I have shared with you, her birth story – which was the most beautiful experience.

